Why kids are getting obese
Hey all, greetings from Santa Monica!
Vitamin Z is a newsletter about health and wellness. If you are new, you can join here. Please comment below with feedback on today’s newsletter.
You can also read this in your browser here.
👦🏻 When I was a kid, my diet was horrible. I ate nothing but pizza and chicken fingers. I hoarded candy like an inmate hoards cigarettes. It wasn’t until my teenage years that I started eating a healthier diet and playing competitive sports.
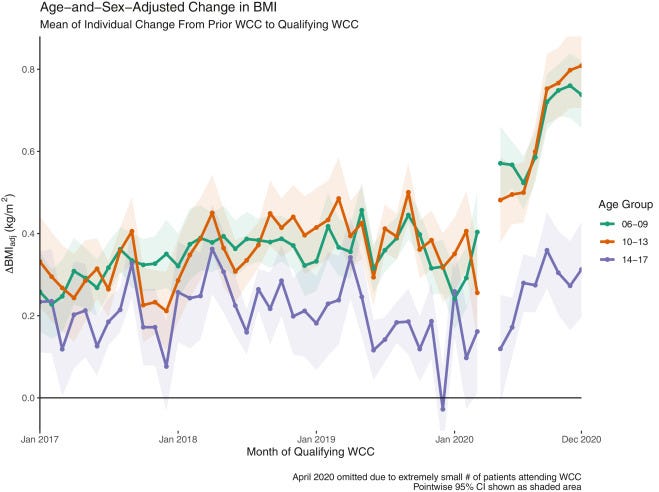
I reflected on this in light of a recent study that childhood obesity has risen sharply during the pandemic. CDC research shows body mass index (BMI) among young people increased between March and November 2020 at nearly double the rate that it did before the pandemic began.
A study from The Lancet found that the weight gain was greater for certain demographic subgroups, including Hispanic, African American and low-income children.
🩺 For this issue I spoke with three healthcare providers who focus on children and nutrition:
Dr. Nancy Rahnama, an LA-based clinical nutritionist board certified in internal medicine and obesity medicine
Dr. Bryan Kalil, a pediatrician based in Texas
Carley Moran, MS, RD, CSCS, a registered dietitian and nutritionist in LA who specializes in sports nutrition and eating disorders
These experts gave me insight into what’s causing rising obesity in young people, and what we can do to help.
In this post I’ll examine the root causes: mental health challenges, socioeconomic issues, the role of parents and schools, screen time and digital addiction. Finally, I’ll share what I’ve learned about a few promising new programs aimed at combating childhood obesity.
🍏 Why should we care about childhood obesity?
When I started doing research on this topic, I knew I needed to approach it with sensitivity. I’m not a parent. Child obesity is a touchy subject. I’m not here to lecture parents.
Losing weight is extremely challenging for most people. No one should be fat-shaming or making people feel bad about themselves. Eating disorders like anorexia are deadly.
That said, obesity is a huge problem in the US. Half of this country is diabetic or pre-diabetic. Yes, the pandemic has been hard on everyone. But the healthcare providers I spoke to believe using food as comfort is not a healthy coping strategy.
Childhood obesity can lead to diabetes, high blood pressure, and heart disease. It causes breathing problems, such as asthma and sleep apnea. Childhood obesity is also related to psychological problems such as anxiety, depression, and low self-esteem.
One of my friends, a doctor, did research on adolescent obesity in San Antonio. She said: “We found that fat kids become fat adults. That is a problem and shouldn’t be ignored.”
A Bill & Melinda Gates Foundation study found that most deaths in the US are preventable and related to nutrition. Poor diets kill nearly twice as many Americans as smoking. Obesity is one of the main risk factors for death from Covid.
The roots of the epidemic
Some of the causes of rising obesity are obvious: people are getting less physical activity during lockdown. They’ve used food as a coping mechanism. Other causes are less obvious: mental health challenges, digital addiction, the role of parents and schools. Let’s explore each one individually.
🍫 Stress eating
The experts I spoke to underscored the challenges of staying fit over the past 18 months:
“Kids are sitting all day, they’re not walking to school,” said Dr. Rahnama. “One thing that helped was school meals. Now they’re depressed from a lack of social interaction, and they’re in front of a computer all day long. Food has always been a source of comfort. It’s a bad combo.”
When you don’t have control of many aspects of life, it’s understandable that people use food to relieve stress or give themselves a feeling of control.
“People are stressed,” said Carley. “What are they supposed to do? Food gives them a pleasure response in the brain, and it seems better than drugs or sex.”
Dr. Kalil says he’s seen many kids with a dramatic increase in weight gain at his practice in North Texas:
“Kids have put on 10, 15, 18 pounds—more than the average kid should gain, which may be 4 or 5 pounds a year. We’ve seen double the average weight gain in the last 18 months.”
🍩 Talking to kids about food
Lockdowns had a significant mental health impact on children, said Dr. Kalil. He’s seen more children with depression, anxiety, and psychotic disorders since Covid.
The emotional distress of being isolated and doing online schooling contributed to disordered eating, said Dr. Rahnama:
“You shouldn’t have to tell an 8-year-old to have only one sugary snack a day. When you restrict foods, it leads to bingeing. Kids will do it in secret and overdo it because they feel like they’re restricted at home.”
Having parents force food on kids can be detrimental to their relationship, said Carley: “Kids with disordered eating will eat junk food secretly when they’re isolated.”
Dr. Rahnama highlighted the challenges of talking to children about their eating habits: “There’s a fine line. At what point am I creating an eating disorder by telling an 8-year-old they should stop eating something?”
Body shaming is a real problem for children and can lead to deadly eating disorders like bulimia or anorexia. Carley said:
“We shouldn’t make kids feel bad for gaining weight during a global pandemic when the whole world is told to stay indoors. This type of body shaming will negatively impact their relationship to food, and can increase their risk for disordered eating behavior.”
📱 More screen time, less green time
One unsurprising result of lockdowns: People were less physically active. Playgrounds were closed. There weren’t as many opportunities to move around.
Digital media and mobile devices contribute to kids not exercising, says Dr. Kalil:
“Kids spend 12 hours a day in front of screens. There’s a greater desire to be on their phones and play video games than to play sports. By age eight or nine, fewer kids at school are trying out for athletic teams. They’re happier staying home playing video games.”
🍔 Fast food nation
We know fast food and ultra-processed foods are linked to obesity. The pandemic worsened this problem as school lunches—a primary source of nutrition for millions of kids in the US—disappeared.
Dr. Kalil said:
“Where we live in North Texas, people eat predominantly fast foods. Most people don’t eat whole foods. The excuse is, parents work so much they don’t have time to cook a decent meal. Fast foods are a big issue. Not enough children are playing sports or exercising to counter the caloric intake.”
I spoke to Nicole Landers, co-founder of LA Children’s Garden. She has worked as a garden educator in low-income communities such as Watts, Los Angeles. She said food access is a big challenge for these communities:
“Within a 5-mile radius in Watts, in South Los Angeles, there are more fast-food restaurants than grocery stores with healthy food options. When you see McDonalds has dollar burgers, dollar sodas and fries, and you can feed your family of four for four dollars, what are you going to serve them?
If you’re a struggling parent, trying to put food on the table with little money, even with SNAP money from the government, it’s not enough.”
Millions of Americans live in so-called food deserts with limited access to whole foods. Obesity is driven by lack of access to healthy foods in poorer communities and the ubiquity of junk food and sugary drinks.
Dr. Kalil said, “There’s hardly a product you can buy that doesn’t have a refined sugar in it. Everything is contaminated with it. I don’t know how you start the process of re-educating. It will require a whole rehabilitation of the American population at large.”
What’s the solution?
1. 🥬 Improving access to healthy food
Health and wellness doesn’t happen in the doctor’s office; it happens in the communities where we live and the environments we grow up in. We can’t address our health challenges until we address the food systems that underlie disease.
Nicole told me about California non-profits and local government programs dedicated to expanding access to healthy foods:
Food Forward is an LA organization on a mission to reduce food waste and increase access to healthy fruits and vegetables through food recovery. The group gathers produce that’s left over from big LA-area farms and produce distributors, takes the leftovers and distributes them in distressed areas.
Cedars-Sinai Hospital offers mobile nutritional workshops for underserved communities in LA.
The city of Oakland created a centralized lunchroom program that distributes fresh, healthy lunches to all Oakland schools. The program provided 11 million meals to families during the pandemic.
2. 👪 Supporting parents
The pandemic has been hard on parents. They’ve had to juggle work, childcare, online learning, and still find time to put food on the table. Many parents work long hours and don’t have time to cook. Kids are allowed to fall into bad eating habits.
Dr. Kalil said parents should set guidelines for diet and nutrition: “You don’t want to create more anxiety, turn the kid into someone with phobias or eating disorders like anorexia. But I think parents are there to set guidelines, and we as a society need to set norms, about what you eat and how much you eat.”
Educating parents is the number-one priority for nutritionists working with children, said Dr. Rahnama:
“We need parents to create boundaries and be firm with those rules. Not just say, it’s ok your kid is chubby, they’ll grow out of it. No, they’re pre-diabetic. Kids are developing sleep apnea.”
Parents should understand the long-term health consequences of childhood obesity, said Dr. Kalil. He said he sees patients who at 30 years old are hypertensive and pre-diabetic with thyroid problems:
“Parents need to be giving their children some guidance. They don’t want to traumatize their kids. The real trauma is coming later. All you’re doing is delaying the trauma that’s coming later in life with chronic illness.”
Carley highlighted the importance of sit-down family meals:
“Prioritize family meals. If you have kids living with you, making an effort to schedule time with others in a formal setting is the number one thing that’s been lost. Parents should make whole foods very available and convenient. Keep a bowl of fruit on the table. Assign children the task of cutting vegetables, if they’re old enough to handle a knife.”
Dr. Rahnama recommends that parents of overweight children start with simple interventions, like eliminating soda:
“The first thing we do is take away any drinks that have calories. Don’t let kids have sugary drinks. There’s a lot more soda intake in low-income families. That’s the best intervention to reduce caloric intake without creating an eating disorder.
Make the small changes where you can, without taking away the three core meals a growing child needs. Take away the excess caloric intake and increase physical activity.”
3. 👩🏫 Empowering schools
Nicole, co-founder of LA Children’s Garden, said we need more school programs focused on health and wellness education. She highlighted the impact of giving students access to gardens:
“If every school could have a garden program to get kids out of the classroom, growing their own kale and arugula, they’ll eat it.
Before we started our garden program in LA, these kids didn’t even know what kale and arugula looked like. Now they’ll bring it home and eat it at home. We proved that. We taught them how to cook it with healthy recipes around their families’ background and culture.”
Teaching a kid how to garden can have a profound impact on their health and well-being, said Nicole:
“If a child says, Mom, I grew this kale at school and I want to eat it, then the kids are teaching the parents. I think that’s a better way for it to happen, because then the child will push their parents to eat that way. From middle school to high school kids, that’s what we’ve seen happen.”
Physical fitness programs at schools should expand beyond traditional P.E., said Dr. Kalil. He stressed the importance of sports programs that get kids’ cardiovascular system going, teach them about good health and get them excited about fitness.
From gardening, to nutrition education, to physical fitness: We can study which school health programs are most effective, and replicate them nationwide to support our children.
Nicole said:
“It comes down to money and access. We need big companies like Nike to step up and give money to education and helping schools in need. Communities are stepping up and taking care of themselves, not waiting for someone else to figure it out.”
Childhood obesity is a bit like climate change: A huge, complex problem with many causes. We’re not going to solve it overnight. My hope is that by shining a light on the roots of the problem, and studying the interventions and programs that work, we can find ways to move toward possible solutions.
Thank you for reading. Until next week,
By Daniel Zahler
Every week I write an email newsletter with perspectives on health and wellness trends, and strategies & tactics on how to optimize cognitive, physical and emotional health. I hold a JD and BA from Harvard, have worked at Goldman Sachs and McKinsey, and advise global business leaders as a GLG council member.
Check out my articles in Thrive Global here.
Enjoy this?
There are a few things to do:
Follow me on Twitter.
Hit reply with your feedback and ideas :)
Share this post with others.